As far as I know, I had never been feared simply for being me, apart from anything I was doing. White, 5’9”, 155 pounds, I don’t cut an especially intimidating figure. What’s more, I usually do what I can to signal that there is no reason to fear me. Walking on empty city streets at night, for example, I cross to the other side or at least keep my distance if I think my approach might frighten someone. But when I was diagnosed with COVID-19, there was nothing I could do to keep people from fearing me. It was the closest I’d ever been to experiencing social stigmatization, though I don’t pretend it was anything like the much worse stigmatizations that other Americans face—for example, “living while black.”
My bout with the virus was relatively mild. I recovered quickly and easily. It helped that I am relatively young (forty-seven), that I don’t have any underlying medical conditions, and that I have regular health care, underwritten by employer-subsidized health insurance. My fever never climbed above 100 degrees and lasted no more than a day. My cough, which I had mistaken for a symptom of seasonal allergies, lasted for only a few days and went away with my fever. I had a feeling of tightness in my chest for a few weeks, but this was never excruciating, only uncomfortable; and I never had any trouble breathing. My energy was quite low for a couple weeks, but it slowly returned. Post-viral acid reflux was more persistent, but it too began to fade after a month—though not before prompting a worried triage nurse to dispatch me to the emergency room after I’d awakened Easter Monday morning dizzy and likely dehydrated. In the hospital, my EKG was normal; my bloodwork indicated that I had not had a heart attack; my chest X-ray was entirely clear; and my blood-oxygen level was 100 percent. Six hours later, I went home, shaken but deeply grateful and relieved.
In short, I was spared. There are so many horror stories to remind me how much worse it could have been.
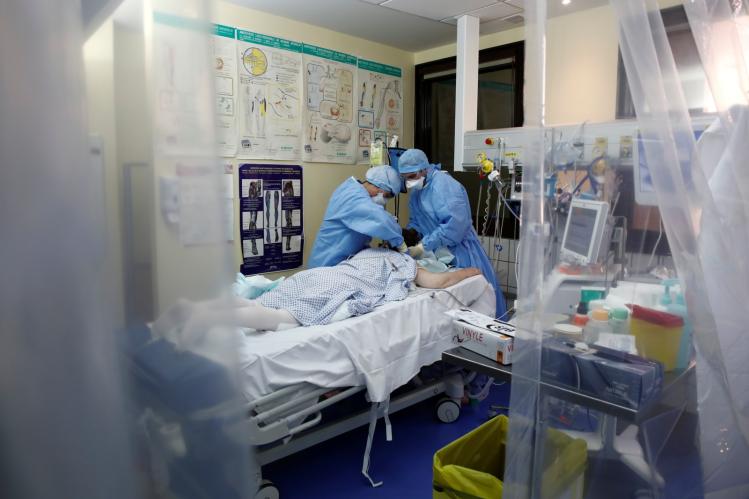
I greatly admire the health-care workers who cared for me during this time. In the COVID-19 testing unit, one of nurses remarked to me, “This is what we’re here for”—though surely he had not anticipated a pandemic when he chose his profession. The nurse who swabbed my nasal cavity was both comforting and professional. The nurses and physicians in the emergency room were competent and clear. Only the person at the registration desk showed any fear, snapping at me that she didn’t want to touch my things when I offered my I.D. and insurance card. In the circumstances of the emergency room, she could be forgiven.
My brush with stigmatization began the following week. At the direction of my primary-care physician, I went to a local clinic for follow-up bloodwork to check my glucose, which the hospital had found to be elevated, likely because of the virus. When I made the appointment by phone and again when I arrived at the clinic, I was asked whether I lived with, or had been in contact with, anyone known to have COVID-19. The best answer seemed to be, “Yes, me!” Nevertheless, the scheduler still made the appointment and the nurse at the door of the clinic still let me into the waiting room. A few minutes later, however, she asked me to go to a different clinic, because the phlebotomist at her clinic was pregnant, and pregnant women may be at higher risk from COVID-19. Off I went. At the second clinic, the nurse at the door would not let me enter the waiting room. Instead, she called her supervisor, who called her supervisor, to figure out what to do with me. Other patients passing by looked at me with suspicion. Twenty minutes later, the nurse told me I could enter.
My primary-care physician also told me to schedule an appointment for a cardiac stress test, to ensure that my chest discomfort was a leftover from the virus and not the symptom of a heart condition. This time, after learning I had tested positive for COVID-19 within the past thirty days, the cardiology office simply refused to see me and canceled my appointment. This got me wondering: Would our health-care system treat former COVID-19 patients anywhere other than in the emergency room or intensive-care unit?
My blood was finally taken after I was allowed into the second clinic’s waiting room, and my stress test was eventually rescheduled for several weeks later. It turns out the health-care system just needed time to get its act together. Some of my acquaintances were slower and more reluctant to believe that I might no longer be contagious—not that I was proposing activities in close quarters anyway. This got me wondering: How long does it take for the scarlet “C” to fade? (Ironically, I was barred from donating blood plasma, presumably teeming with COVID-19 antibodies, because I had lived for a year in England in the early 1990s, which marks me as a potential carrier of Creutzfeldt-Jakob disease. That “C,” at least, may be permanent.)
It’s not that I don’t sympathize with those acquaintances who seem to fear me. Though I’m probably now immune to the virus for at least several months, I still fear it. It made me feel more fragile than I’d ever felt before, and for weeks I was scared of relapse. My dizziness on Easter Monday was surely aggravated by fear that here, at last, was the precipitous decline I had read about: one feels better for a few days and then the virus comes back with a vengeance. I was also anxious that I might have infected a friend with whom I had gone dog-walking a few days before I came down with my fever. She lives with her ninety-year-old father; our shared fear was that the virus would pass from me to her to him. She and I checked in with each other every day during the virus’s normal incubation period. Fortunately, neither she nor anyone in her family developed symptoms.
The trauma experienced by healthcare workers during this pandemic—afraid for themselves, terrified that they might infect loved-ones, devastated by what they see happening to their patients—is only beginning to be documented. Physician suicide rates were already the highest of any profession before the pandemic hit. There is reason to worry that they will now rise even higher.
So-called deaths of despair—deaths from drug overdoses, suicide, and alcohol-related disease—have greatly increased over the past two decades in the United States. For the most part, the spike in midlife mortality and morbidity has been a white, working-class phenomenon, hitting hard in areas like northeastern Pennsylvania, where I live. Who knows what new forms of grief will emerge in the aftermath of the pandemic? A recent story about the awful toll of the virus on working-class people in nearby Hazleton bodes very ill.
Of course, my own experience with the virus colors my reading of the news and my reaction to the rush of some states to “reopen” their economy. I had to step back from correspondence with a friend who bemoaned our country’s “mental fragility” in the face of the pandemic and claimed that the whole thing is nearing “hoax proportions.” Sorry, but you don’t want this disease. It’s much more lethal than the flu, and even if it’s not especially bad for you (as it wasn’t for me), it is life-threatening to many others. African-Americans and Hispanics have been hit disproportionately hard by the virus, as have the elderly and those with “comorbidities.”
That said, I am perhaps more nervous than I should be with, for example, allowing my children to see friends—generally with masks and six feet apart—as our county relaxes its restrictions. The friend who lamented our mental fragility directed me to a sermon that C. S. Lewis preached at Oxford in 1939, “Learning in War-Time.” Lewis appeals to his listeners to heed the voice of reason and to quiet “the voice of our nerves and our mass emotions.” He goes on, in terms that sound at first contemporary, “Life has never been normal. Even those periods which we think most tranquil, like the nineteenth century, turn out, on closer inspection, to be full of cries, alarms, difficulties, emergencies.”
Point taken, but what follows? Lewis argued for “leaving futurity in God’s hands” and urged students who had been sent up to Oxford to focus on the task at hand—namely, learning. Unless a vaccine is developed amazingly quickly, it seems the task at hand for us, here and now, is also learning, but in a different sense from what Lewis meant. In the teeth of an economic depression, with riots in our city streets, we need to learn how to negotiate life with people who have quite different understandings of the risks of COVID-19, quite different levels of tolerance for risk, and quite different levels of tolerance for one another. Maybe I’m wrong, but book-learning in a time of war seems much easier.


